Right Hemispheric Stroke - General Information
What is a right hemispheric stroke?
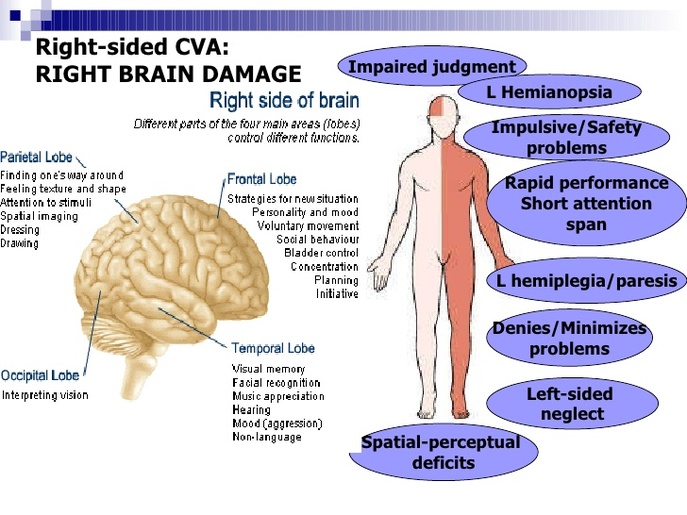
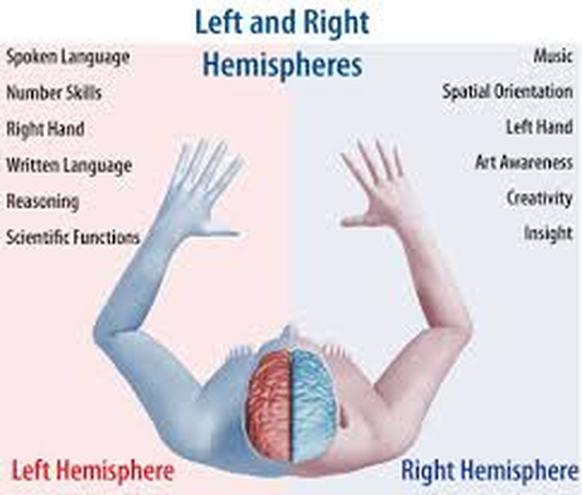
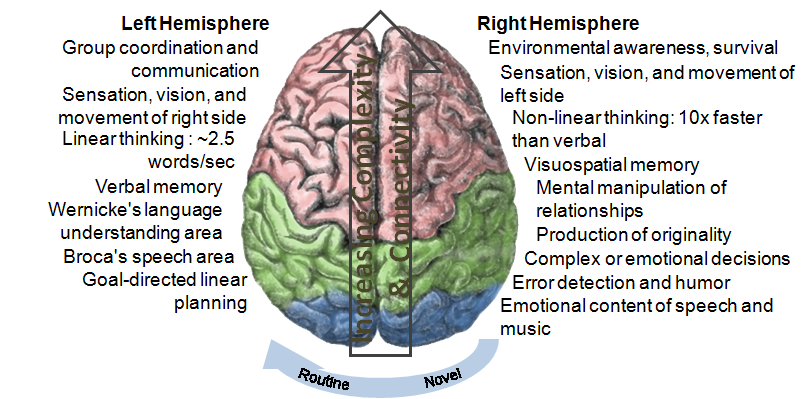
A stroke occurs when blood cannot flow to your brain. The right side (hemisphere) of your brain controls the left side of your body. It may also affect your speech and language abilities.
What causes a right hemispheric stroke?
What are the signs and symptoms of a right hemispheric stroke?
A stroke occurs when blood cannot flow to your brain. The right side (hemisphere) of your brain controls the left side of your body. It may also affect your speech and language abilities.
What causes a right hemispheric stroke?
- Ischemic stroke: An artery to your brain gets blocked, usually by a blood clot. The clot stops blood and oxygen from reaching your brain.
- Hemorrhagic stroke: A blood vessel breaks and leaks because a clot gets stuck in it, or the vessel wall is weak. Blood then flows out of the vessel and into brain tissue.
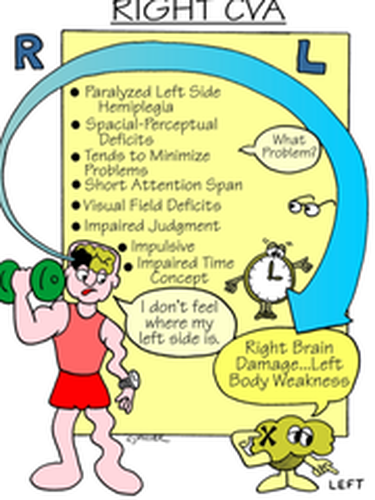
What are the signs and symptoms of a right hemispheric stroke?
- Difficulty remembering, impulsive behavior, or mood changes
- Paralysis on 1 or both sides of your body
- Trouble walking, or falling toward your left side
- Lack of awareness of the left side of your body
- Trouble swallowing, speaking, reading, writing, or understanding language
- Changes in mood or the ability to pay attention or solve problems
What increases my risk of a right hemispheric stroke?
- Age 55 or older
- Male or African-American
- Physical inactivity or obesity
- High cholesterol, high blood pressure, or diabetes
- Smoking
- Chronic inflammatory disease, such as rheumatoid arthritis or lupus
- Family history of stroke, or a low birthweight
- Heart conditions, such as atrial fibrillation, myocardial infarction, or valve disease
- Birth control pills or hormone replacement medicine
- Pregnancy or delivery within the past 6 weeks
How is a right hemispheric stroke diagnosed?
Your healthcare provider will ask about your symptoms and when they started. He will look for signs that show which part of your brain was injured. You may need any of the following:
- A CT or MRI may show where the stroke happened and any damage you have. You may be given contrast liquid to help your skull and brain show up better in the pictures. Tell the healthcare provider if you have ever had an allergic reaction to contrast liquid. Do not enter the MRI room with anything metal. Metal can cause serious injury. Tell the healthcare provider if you have any metal in or on your body.
- An arteriography is used to take x-rays of your arteries to look for blood flow blockage.
- A carotid ultrasound may show narrow or blocked carotid arteries. The carotid arteries are blood vessels in your neck that carry blood to your brain.
How is a right hemispheric stroke treated?
- Medicines may help improve your blood's ability to clot and stop the bleeding. You may instead need medicine to break up blood clots, or to prevent them from forming. The type of medicine you receive depends on what is causing your stroke. You may also need medicine for high blood pressure, high cholesterol, or diabetes.
- Physical and occupational therapy may be needed. A physical therapist teaches you exercises to help improve movement and strength, and to decrease pain. An occupational therapist teaches you skills to help with your daily activities.
- Surgery may be needed to place a tube in your skull. The tube drains extra fluid and checks the pressure in your brain.
How can I decrease my risk for a stroke?
- Manage health conditions. Take your medicine as directed. Check your blood pressure and blood sugar levels as directed. Keep a record and bring it to your follow-up visits.
- Eat a variety of healthy foods. Healthy foods include whole-grain breads, low-fat dairy products, beans, lean meats, and fish. Eat at least 5 servings of fruits and vegetables each day. Choose foods that are low in fat, cholesterol, salt, and sugar. Eat foods that are high in potassium, such as potatoes and bananas.
- Maintain a healthy weight. Ask your healthcare provider how much you should weigh. Ask him to help you create a weight loss plan if you are overweight. Ask about the best exercise plan for you.
- Limit or do not drink alcohol. Limit alcohol to 2 drinks per day if you are a man. Limit alcohol to 1 drink per day if you are a woman. A drink of alcohol is 12 ounces of beer, 5 ounces of wine, or 1½ ounces of liquor.
- Do not smoke cigarettes or use street drugs. Smoking and drugs increase your risk for a stroke. Ask your healthcare provider for information if you need help quitting.
- Get a flu vaccine. To prevent influenza (flu), all adults should get the influenza vaccine. Get the vaccine every year as soon as it becomes available.
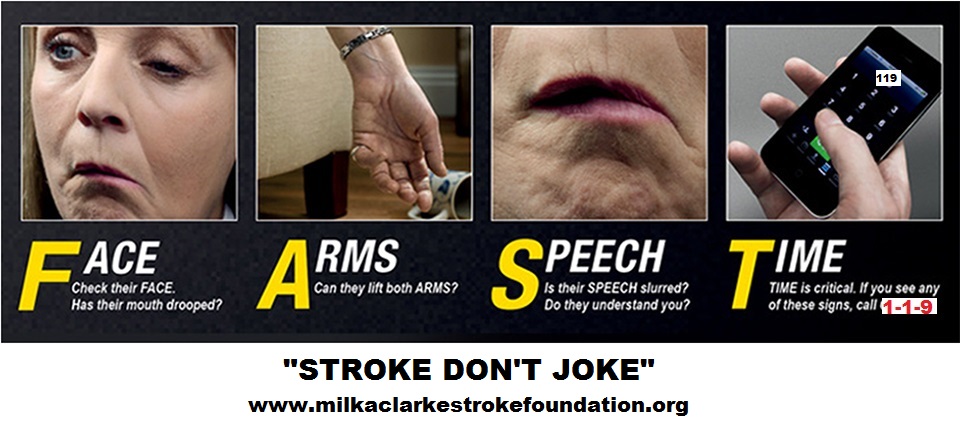
How can I tell if someone is having a stroke? Know the F.A.S.T. test to recognize the signs of a stroke:
- F = Face: Ask the person to smile. Drooping on 1 side of the mouth or face is a sign of a stroke.
- A = Arms: Ask the person to raise both arms. One arm that slowly comes back down or cannot be raised is a sign of a stroke.
- S = Speech: Ask the person to repeat a simple sentence that you say first. Speech that is slurred or sounds strange is a sign of a stroke.
- T = Time: Call 119 if you see any of these signs. This is an emergency. The person should be taken to the hospital immediately.
Call 119 for any of the following:
- You have a seizure.
- You feel lightheaded, short of breath, and have chest pain.
- You cough up blood.
- You have weakness or numbness in your arm, leg, or face.
- You are confused and have problems speaking or understanding speech.
- You have a severe headache, or loss of balance or coordination.
When should I seek immediate care?
- You have double vision or vision loss.
- You are bleeding from your rectum or nose.
- Your arm or leg feels warm, tender, and painful. It may look swollen and red.
When should I contact my healthcare provider?
- Your blood pressure is higher or lower than you were told it should be.
- You have questions or concerns about your condition or care.
While you are hospitalized
CARE AGREEMENT:
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your caregivers to decide what care you want to receive. You always have the right to refuse treatment.
RISKS:
You may get blood clots that can break loose and travel to your lungs or brain. You may have another stroke or go into a coma. You may be paralyzed on one or both sides of your body. You may not be able to care for yourself or live alone. You are at greater risk for falling. You may develop muscle shortening or bedsores. Even with treatment, you may have lasting problems talking, thinking, or moving your body. Without treatment, your risk for another stroke increases. This can be life-threatening.
WHILE YOU ARE IN THE HOSPITAL:
Informed consent is a legal document that explains the tests, treatments, or procedures that you may need. Informed consent means you understand what will be done and can make decisions about what you want. You give your permission when you sign the consent form. You can have someone sign this form for you if you are not able to sign it. You have the right to understand your medical care in words you know. Before you sign the consent form, understand the risks and benefits of what will be done. Make sure all your questions are answered.
An IV is a small tube placed in your vein that is used to give you medicine or liquids.
Tests:
CARE AGREEMENT:
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your caregivers to decide what care you want to receive. You always have the right to refuse treatment.
RISKS:
You may get blood clots that can break loose and travel to your lungs or brain. You may have another stroke or go into a coma. You may be paralyzed on one or both sides of your body. You may not be able to care for yourself or live alone. You are at greater risk for falling. You may develop muscle shortening or bedsores. Even with treatment, you may have lasting problems talking, thinking, or moving your body. Without treatment, your risk for another stroke increases. This can be life-threatening.
WHILE YOU ARE IN THE HOSPITAL:
Informed consent is a legal document that explains the tests, treatments, or procedures that you may need. Informed consent means you understand what will be done and can make decisions about what you want. You give your permission when you sign the consent form. You can have someone sign this form for you if you are not able to sign it. You have the right to understand your medical care in words you know. Before you sign the consent form, understand the risks and benefits of what will be done. Make sure all your questions are answered.
An IV is a small tube placed in your vein that is used to give you medicine or liquids.
Tests:
- A CT or MRI may show where the stroke happened and any damage you have. You may be given contrast liquid to help your skull and brain show up better in the pictures. Tell the healthcare provider if you have ever had an allergic reaction to contrast liquid. Do not enter the MRI room with anything metal. Metal can cause serious injury. Tell the healthcare provider if you have any metal in or on your body.
- An arteriography is used to take x-rays of your arteries to look for blood flow blockage.
- Frequent blood tests may be needed while you are being treated for your stroke. These tests can tell healthcare providers if you are getting the right amount of medicine.
- A carotid ultrasound uses sound waves to show the blood flow in your carotid arteries. The carotid arteries are blood vessels in your neck that carry blood to your brain. A carotid ultrasound checks for narrow or blocked carotid arteries.
- A swallow study is used to take x-rays as you swallow certain foods and drinks. This test shows if food and liquids travel to your stomach correctly.
Monitoring:
Medicines may help improve your blood's ability to clot and stop the bleeding. You may instead need medicine to break up blood clots, or to prevent them from forming. The type of medicine you receive depends on what is causing your stroke. You may also need medicine for high blood pressure, high cholesterol, or diabetes.
Treatment:
Follow up with your healthcare provider or neurologist as directed: You may need to come in for regular tests of your brain function. You may also need regular blood tests. Write down your questions so you remember to ask them during your visits.
Go to physical or occupational therapy: A physical therapist teaches you exercises to help improve movement and strength, and to decrease pain. An occupational therapist teaches you skills to help with your daily activities.
Prevent another stroke:
- You may need extra oxygen if your blood oxygen level is lower than it should be. You may get oxygen through a mask placed over your nose and mouth or through small tubes placed in your nostrils. Ask your healthcare provider before you take off the mask or oxygen tubing.
- A neuro exam may show how well your brain works after a stroke. Healthcare providers will check how your pupils react to light. They may check your memory and how easily you wake up. Your hand grasp and balance may also be tested.
- Intake and output may need to be measured. Healthcare providers may measure how much liquid you are getting and how much you are urinating.
- A ventilator is a machine that gives you oxygen and breathes for you when you cannot breathe well on your own. An endotracheal (ET) tube is put into your mouth or nose and attached to the ventilator. You may need a trach if an ET tube cannot be placed. A trach is a tube put through an incision and into your windpipe.
- An ICP monitor measures the pressure inside your skull. A small tube is put through your skull and connected to a screen.
Medicines may help improve your blood's ability to clot and stop the bleeding. You may instead need medicine to break up blood clots, or to prevent them from forming. The type of medicine you receive depends on what is causing your stroke. You may also need medicine for high blood pressure, high cholesterol, or diabetes.
Treatment:
- You may need to wear pressure stockings or inflatable boots. The stockings are tight and put pressure on your legs. The boots have an air pump that tightens and loosens different areas of the boots. This improves blood flow and helps prevent clots.
- Physical and occupational therapy may be needed. A physical therapist teaches you exercises to help improve movement and strength, and to decrease pain. An occupational therapist teaches you skills to help with your daily activities.
- Bladder and bowel training helps you control when you urinate or have a bowel movement.
- Swallow therapy may help you learn safe ways to swallow to prevent coughing and choking.
- A feeding tube may be needed if you cannot swallow food or liquids.
- Surgery may be needed to place a tube in your skull. The tube drains extra fluid and checks the pressure in your brain.
Follow up with your healthcare provider or neurologist as directed: You may need to come in for regular tests of your brain function. You may also need regular blood tests. Write down your questions so you remember to ask them during your visits.
Go to physical or occupational therapy: A physical therapist teaches you exercises to help improve movement and strength, and to decrease pain. An occupational therapist teaches you skills to help with your daily activities.
Prevent another stroke:
- Manage health conditions. Take your medicine as directed. Check your blood pressure and blood sugar levels as directed. Keep a record and bring it to your follow-up visits.
- Eat a variety of healthy foods. Healthy foods include whole-grain breads, low-fat dairy products, beans, lean meats, and fish. Eat at least 5 servings of fruits and vegetables each day. Choose foods that are low in fat, cholesterol, salt, and sugar. Eat foods that are high in potassium, such as potatoes and bananas.
- Maintain a healthy weight. Ask your healthcare provider how much you should weigh. Ask him to help you create a weight loss plan if you are overweight. Ask about the best exercise plan for you.
- Limit or do not drink alcohol. Limit alcohol to 2 drinks per day if you are a man. Limit alcohol to 1 drink per day if you are a woman. A drink of alcohol is 12 ounces of beer, 5 ounces of wine, or 1½ ounces of liquor. It is best if you strop drinking completely.
- Do not smoke cigarettes or use street drugs. Smoking and drugs increase your risk for a stroke. Ask your healthcare provider for information if you need help quitting.