Dos and Don’ts While Waiting for an Ambulance
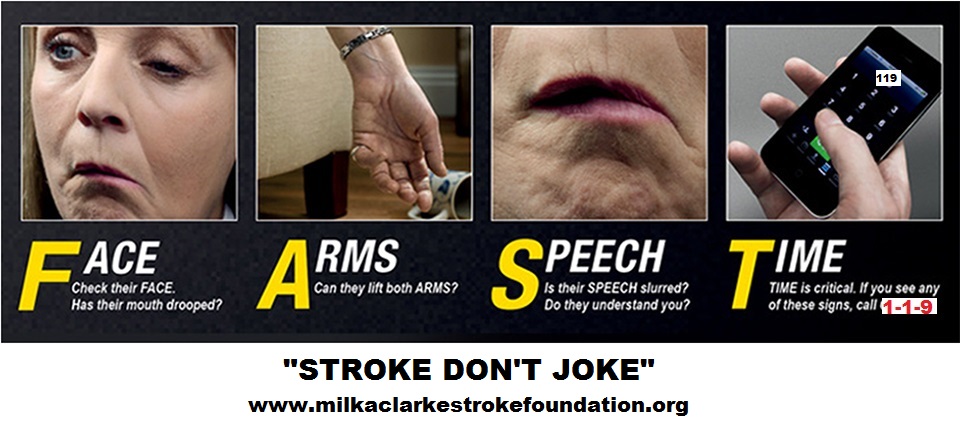
Your friend is over for dinner. She’s sitting at the table, fork in hand. All of a sudden, she drops the fork and she looks scared. You ask her what’s wrong, but she’s having trouble talking. You notice that one side of her body appears to be weak, and her mouth is drooping. You know what that means; she’s had a stroke.
You immediately call 119. But you don’t know what you to do while the ambulance is on its way. Is there anything you can do to help your friend? Or should you just wait until the paramedics arrive?
It’s important to be prepared for a medical emergency. Read on to find out what you should and shouldn’t do while you’re waiting for help.
Do:
You immediately call 119. But you don’t know what you to do while the ambulance is on its way. Is there anything you can do to help your friend? Or should you just wait until the paramedics arrive?
It’s important to be prepared for a medical emergency. Read on to find out what you should and shouldn’t do while you’re waiting for help.
Do:
- Use the word “stroke” when you call 119.
- Tell the 119 operator where you are if you’re calling from a cell phone in case the call drops. You should also give the operator your cell phone number.
- Stay on the line with the 911 operator and follow his or her instructions.
- Keep the person safe. If she’s conscious, place her on her side. Her head should be slightly raised and supported.
- Loosen clothing that could get in the way of breathing.
- Note the time. This is important information for doctors. Most strokes are caused by blood clots. The clot-busting medication tissue plasminogen activator (tPA) can only be given within a few hours of the start of symptoms.
- Tell emergency responders what you saw and heard. Describe your friend’s symptoms.
- Stay with her. Your friend will be scared.
- Remain calm.
- If your friend is unconscious, check her pulse and her breathing and start CPR. If you’re unsure how to do that, the 911 operator will walk you through it.
- Unlock the front door so paramedics can get in quickly. The 911 operator may tell you to do that or tell you to open the front door ahead of time. With stroke, the sooner the patient receives treatment, the better the chances of survival and recovery.
- Drive her to the hospital yourself. A stroke is a medical emergency. Paramedics will let doctors in the emergency room know they are on their way with someone who has had a stroke. The hospital will prepare for the arrival ahead of time.
- Give her anything to eat or drink. This could cause her to choke.
- Give her any medication, including aspirin.
Debunking Stroke Myths
Four out of five strokes are preventable. Positive diet and lifestyle changes, as well as regular exercise and quitting smoking can all decrease stroke risk significantly.
And yet, a common myth is that strokes can’t be prevented.
Even more myths about the disease that affects 800,000 people each year exist. Here are a few prevalent misconceptions about stroke debunked.
Myth: Strokes don’t affect people under the age of 65.
Strokes don’t discriminate based on age. A quarter of strokes occur in people younger than 65, and one in ten strokes occur in people age 45 and younger, and those numbers are rising.
Myth: Recovery only happens in the first few months after a stroke occurs.
Although the time shortly after a stroke occurs is important, most stroke survivors see the effects of recovery for the rest of their lives. Continuing physical, speech, and occupational therapy for years after a stroke can still yield positive results.
Myth: Stroke happens in the heart.
Strokes occur when blood supply to a portion of the brain is cut off.
Myth: If you’re not in pain, it’s not a stroke.
Many stroke patients don’t feel any pain at all. The more common symptoms include dizziness and loss of balance, difficulty speaking, numbness in extremities, and trouble understanding those around you.
Myth: Strokes don’t run in the family.
The risk of having a stroke increases for those with a family history of stroke.
Myth: Strokes are rare.
There are 7 million stroke survivors in the United States and stroke is the fifth leading cause of death in the country.
Myth: Small strokes don’t need medical attention.
Every stroke requires immediate medical attention. Prompt treatment could be the difference between life and death and making a full recovery versus having severe, long-term effects.
Myth: Stroke survivors have no life for themselves.
Although many survivors live with the effects of stroke for the rest of their lives, many make a strong recovery and live a fulfilling life. After suffering a stroke at age 21, survivor Andrew Bloom of West Palm Beach, Fla., graduated from college, got married, and had two kids. Bert Seitzinger of Virginia lost most of the use in his left hand after a stroke six years ago, but now spends his time restoring vehicles and building items by hand. “Challenges do not limit your ability to have a normal life,” Bloom says.
And yet, a common myth is that strokes can’t be prevented.
Even more myths about the disease that affects 800,000 people each year exist. Here are a few prevalent misconceptions about stroke debunked.
Myth: Strokes don’t affect people under the age of 65.
Strokes don’t discriminate based on age. A quarter of strokes occur in people younger than 65, and one in ten strokes occur in people age 45 and younger, and those numbers are rising.
Myth: Recovery only happens in the first few months after a stroke occurs.
Although the time shortly after a stroke occurs is important, most stroke survivors see the effects of recovery for the rest of their lives. Continuing physical, speech, and occupational therapy for years after a stroke can still yield positive results.
Myth: Stroke happens in the heart.
Strokes occur when blood supply to a portion of the brain is cut off.
Myth: If you’re not in pain, it’s not a stroke.
Many stroke patients don’t feel any pain at all. The more common symptoms include dizziness and loss of balance, difficulty speaking, numbness in extremities, and trouble understanding those around you.
Myth: Strokes don’t run in the family.
The risk of having a stroke increases for those with a family history of stroke.
Myth: Strokes are rare.
There are 7 million stroke survivors in the United States and stroke is the fifth leading cause of death in the country.
Myth: Small strokes don’t need medical attention.
Every stroke requires immediate medical attention. Prompt treatment could be the difference between life and death and making a full recovery versus having severe, long-term effects.
Myth: Stroke survivors have no life for themselves.
Although many survivors live with the effects of stroke for the rest of their lives, many make a strong recovery and live a fulfilling life. After suffering a stroke at age 21, survivor Andrew Bloom of West Palm Beach, Fla., graduated from college, got married, and had two kids. Bert Seitzinger of Virginia lost most of the use in his left hand after a stroke six years ago, but now spends his time restoring vehicles and building items by hand. “Challenges do not limit your ability to have a normal life,” Bloom says.