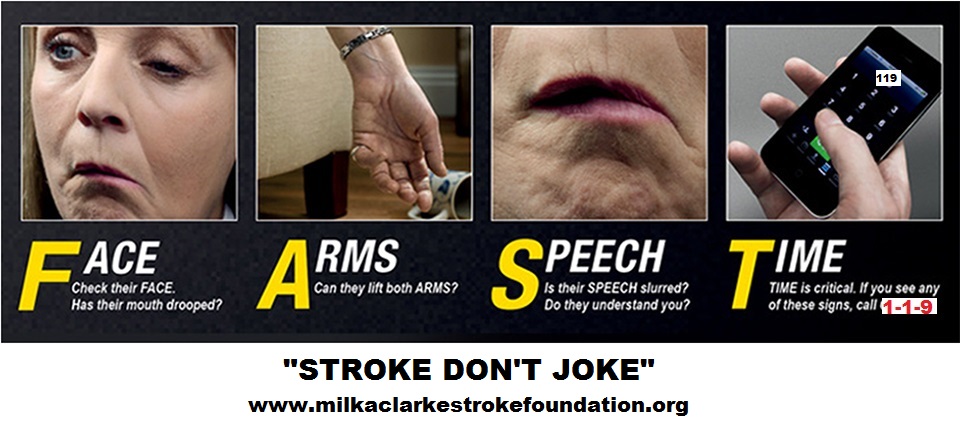
Why a dysphagia diet is needed
- Stroke
- Severe dental problems
- Conditions that lead to less saliva, such as Sjogren syndrome
- Mouth sores
- Parkinson disease or other neurologic conditions
- Muscular dystrophies
- Blockage in the esophagus, such as a growth from cancer
You may need to follow a dysphagia diet for only a short time. Or you may be on it for a while. It depends on what is causing your dysphagia and how serious it is. A speech-language pathologist (SLP) assesses a person with dysphagia. The SLP will determine your risk for aspiration and talk about the best food and drink choices for you.
Levels of a dysphagia diet
The Academy of Nutrition and Dietetics has created a diet plan for people with dysphagia. The plan is called the National Dysphagia Diet. The dysphagia diet has 4 levels of foods. The levels are:
- Level 1. These are foods that are pureed or smooth, like pudding. They need no chewing. This includes foods such as yogurt, mashed potatoes with gravy to moisten it, smooth soups, and pureed vegetables and meats.
- Level 2. These are moist foods that need some chewing. They include soft, cooked, or mashed fruits or vegetables, soft or ground meats moist with gravy, cottage cheese, peanut butter, and soft scrambled eggs. You should avoid crackers, nuts, and other dry foods.
- Level 3. This includes soft-solid foods that need more chewing. This includes meat, fruit, and vegetables that are easy to cut or mash. You should avoid crunchy, sticky, or very dry foods. This includes nuts, crackers, chips, and other snack foods.
- Level 4. This level includes all foods.
You will also need to be careful about the liquids you drink. Talk with your SLP about the liquids that are allowed on your dysphagia diet. Here is more information on managing liquids in a dysphagia diet.
Preparing food and liquids
Your SLP will give you instructions about how to prepare your food. You may need to avoid certain foods, or make changes to some foods. For example, you may need to puree your food. Make sure to taste and season your food before pureeing it. It will be easier to adjust to a new diet if your food smells and tastes appealing.
You may also need to make liquids thicker. You can manage your liquids by making thin liquids thicker. This is done by adding a flavorless gel, gum, powder, or other liquid to it. These are called thickeners. You can also buy pre-thickened liquids. Talk with your SLP if you have any questions about managing your liquids.
While you eat
While eating or drinking, it may help to sit upright, with your back straight. You may need support pillows to get into the best position. It may also help to have few distractions while eating or drinking. Changing between solid food and liquids may also help your swallowing. Stay upright for at least 30 minutes after eating. This can help reduce the risk for aspiration.
Keep watch for symptoms of aspiration such as:
- Coughing or wheezing during or right after eating
- Excess saliva
- Shortness of breath or fatigue while eating
- A wet-sounding voice during or after eating or drinking
- Fever 30 to 60 minutes after eating
After meals, it’s important to do proper oral care. The SLP can give you instructions for your teeth or dentures. Make sure to not swallow any water during your oral care routine.
Checking your health
Your health care team will keep track of how well you are swallowing. You may need follow-up tests such as a fiberoptic endoscopic evaluation of swallowing (FEES) test. If your swallowing gets better or worse, your SLP may change your dysphagia diet over time. In time you may be able to eat and drink foods and liquids of all kinds.
Getting enough liquids
While on a dysphagia diet, you may have trouble taking in enough fluid. This can cause dehydration, which can lead to serious health problems. Talk with your health care team about how you can help prevent this. In some cases drinking thicker liquids may make some of your medicines work less well. Because of this, you may need some of your medicines changed for a while.
While you are on a dysphagia diet
- Follow all instructions about what food and drink you can have.
- Do swallowing exercises as advised.
- Do not change your food or liquids, even if your swallowing gets better. Talk with your health care provider first.
- Crush medicines and mix them with food as needed.
- Tell all health care providers and caregivers that you are on a dysphagia diet. Explain which foods and liquids you can and cannot have.
When to call your health care provider
Call 119 if you have trouble breathing because of food blocking your airway.
Call your health care provider right away if you have any of these:
· Trouble swallowing that gets worse
· Unplanned weight loss
· Chewed food coming back up into the mouth
· Vomiting
 RSS Feed
RSS Feed